ME/CFS Science Blog
Senior Member (Voting Rights)
An old study that is frequently cited in the psychosomatic literature on ME/CFS. Suspect it influenced a lot of people. It concluded that personality and emotional factors influence recovery from Asian flu in the 1950s.
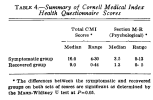
Convalescence from influenza. A study of the psychological and clinical determinants - PubMedIn August of 1957, a total of 600 subjects were administered the MMPI and the CMI.In the winter of 1957-1958, 26 of these persons reported to the dispensary with an acute illness that was diagnosed as influenza.In 19 of these cases, the diagnosis of Asian influenza was confirmed by serological tests or virus isolation.The 26 persons with influenza were divided into two groups: (1) Recovered group, 14 persons, who became asymptomatic 3-14 days with an average of 7.9 days after the onset of the illness, and (2) Symptomatic group, 12 persons, who retained symptoms beyond 3 weeks.These two groups did not differ from each other with respect to clinical characteristics of their acute illness. Significant differences were observed, however, in the psychological test results and are in accord with the prediction, derived from a previously reported study of recovery patterns following acute brucellosis, that delayed recovery following acute self-limited illness occurs in persons who respond to psycho¬logical tests in patterns characteristic of depression-prone patients. Since the psychological data in this study were obtained prior to the illness, the evidence supports the view that this emotional state or attitude is not secondary to the illness, existed prior to it, and in significant measure was a determining factor in delaying symptomatic recovery from acute illness. In addition, itis probable that the somewhat older age ofthe Symptomatic group also contributed to their slower recovery following influenza.