Prevalence and Patterns of Gulf War Illness in Kansas Veterans: Association of Symptoms with Characteristics of Person, Place, and Time of Military Service
Steele, L.
Abstract
Gulf War veterans have reported health problems that they attribute to their military service, but little is understood about the nature or extent of these conditions. To determine whether Kansas Gulf War veterans are affected by excess health problems, a population-based survey of 1,548 veterans who served in the Persian Gulf War (PGW) and 482 veterans who served elsewhere (non-PGW) was conducted in 1998.
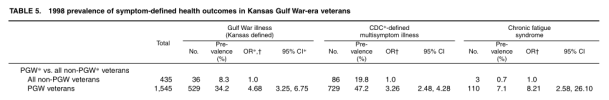
Gulf War illness, defined as having chronic symptoms in three of six domains, occurred in 34% of PGW veterans, 12% of non-PGW veterans who reported receiving vaccines during the war, and 4% of non-PGW veterans who did not receive vaccines.
The prevalence of Gulf War illness was lowest among PGW veterans who served on board ship (21%) and highest among those who were in Iraq and/or Kuwait (42%). Among PGW veterans who served away from battlefield areas, Gulf War illness was least prevalent among those who departed the region prior to the war (9%) and most prevalent among those who departed in June or July of 1991 (41%).
Observed patterns suggest that excess morbidity among Gulf War veterans is associated with characteristics of their wartime service, and that vaccines used during the war may be a contributing factor.
Web | DOI | American Journal of Epidemiology | Paywall
Steele, L.
Abstract
Gulf War veterans have reported health problems that they attribute to their military service, but little is understood about the nature or extent of these conditions. To determine whether Kansas Gulf War veterans are affected by excess health problems, a population-based survey of 1,548 veterans who served in the Persian Gulf War (PGW) and 482 veterans who served elsewhere (non-PGW) was conducted in 1998.
Gulf War illness, defined as having chronic symptoms in three of six domains, occurred in 34% of PGW veterans, 12% of non-PGW veterans who reported receiving vaccines during the war, and 4% of non-PGW veterans who did not receive vaccines.
The prevalence of Gulf War illness was lowest among PGW veterans who served on board ship (21%) and highest among those who were in Iraq and/or Kuwait (42%). Among PGW veterans who served away from battlefield areas, Gulf War illness was least prevalent among those who departed the region prior to the war (9%) and most prevalent among those who departed in June or July of 1991 (41%).
Observed patterns suggest that excess morbidity among Gulf War veterans is associated with characteristics of their wartime service, and that vaccines used during the war may be a contributing factor.
Web | DOI | American Journal of Epidemiology | Paywall