nataliezzz
Senior Member (Voting Rights)
The effect of nasal continuous positive airway pressure on the symptoms of Gulf War illness
Mohammad M. Amin, Morris S. Gold, Joan E. Broderick, Avram R. Gold
https://www.researchgate.net/publication/45695854_The_effect_of_nasal_continuous_positive_airway_pressure_on_the_symptoms_of_Gulf_War_illness (PDF available)
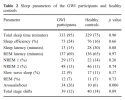
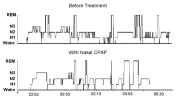
Purpose: We performed a pilot study to determine whether nasal continuous positive airway pressure (CPAP) alleviates the symptoms of veterans with Gulf War illness (GWI) and sleep disordered breathing (SDB).
Methods: Eighteen male veterans with GWI and SDB recruited by advertisement, participated in a randomized, single-masked, sham-controlled treatment trial. Participants received 3 weeks of treatment during sleep with either therapeutic nasal CPAP or sham nasal CPAP. Using validated questionnaires, pain, fatigue, cognitive function, sleep disturbance, and general health were assessed by self-report before and after treatment. One of the participants assigned to therapeutic CPAP was excluded from the trial before starting treatment, leaving 17 participants.
Results: Compared to the nine sham nasal CPAP recipients, the eight participants receiving therapeutic nasal CPAP experienced improvements in pain (34%; p = 0.0008), fatigue (38%; p = 0.0002), cognitive function (33%; p = 0.004), sleep quality (41%; p = 0.0003), physical health (34%; p = 0.0003), and mental health (16%; p = 0.03).
Conclusions: Our findings in this pilot study suggest that nasal CPAP may greatly improve symptoms in veterans with GWI and SDB.
Mohammad M. Amin, Morris S. Gold, Joan E. Broderick, Avram R. Gold
https://www.researchgate.net/publication/45695854_The_effect_of_nasal_continuous_positive_airway_pressure_on_the_symptoms_of_Gulf_War_illness (PDF available)
Purpose: We performed a pilot study to determine whether nasal continuous positive airway pressure (CPAP) alleviates the symptoms of veterans with Gulf War illness (GWI) and sleep disordered breathing (SDB).
Methods: Eighteen male veterans with GWI and SDB recruited by advertisement, participated in a randomized, single-masked, sham-controlled treatment trial. Participants received 3 weeks of treatment during sleep with either therapeutic nasal CPAP or sham nasal CPAP. Using validated questionnaires, pain, fatigue, cognitive function, sleep disturbance, and general health were assessed by self-report before and after treatment. One of the participants assigned to therapeutic CPAP was excluded from the trial before starting treatment, leaving 17 participants.
Results: Compared to the nine sham nasal CPAP recipients, the eight participants receiving therapeutic nasal CPAP experienced improvements in pain (34%; p = 0.0008), fatigue (38%; p = 0.0002), cognitive function (33%; p = 0.004), sleep quality (41%; p = 0.0003), physical health (34%; p = 0.0003), and mental health (16%; p = 0.03).
Conclusions: Our findings in this pilot study suggest that nasal CPAP may greatly improve symptoms in veterans with GWI and SDB.
Last edited by a moderator: