The Long Tail of Long COVID-19: Broad and Extensive Increase in Utilization Within an Integrated Healthcare System
 www.cureus.com
www.cureus.com
Background
The impact of the emergence of Long COVID on healthcare utilization in a U.S. community setting remains underexplored.
Objective
To examine the healthcare utilization of Long COVID patients compared with pre-COVID-19 era controls before and after SARS-CoV-2 infection within a large integrated delivery system.
Methods
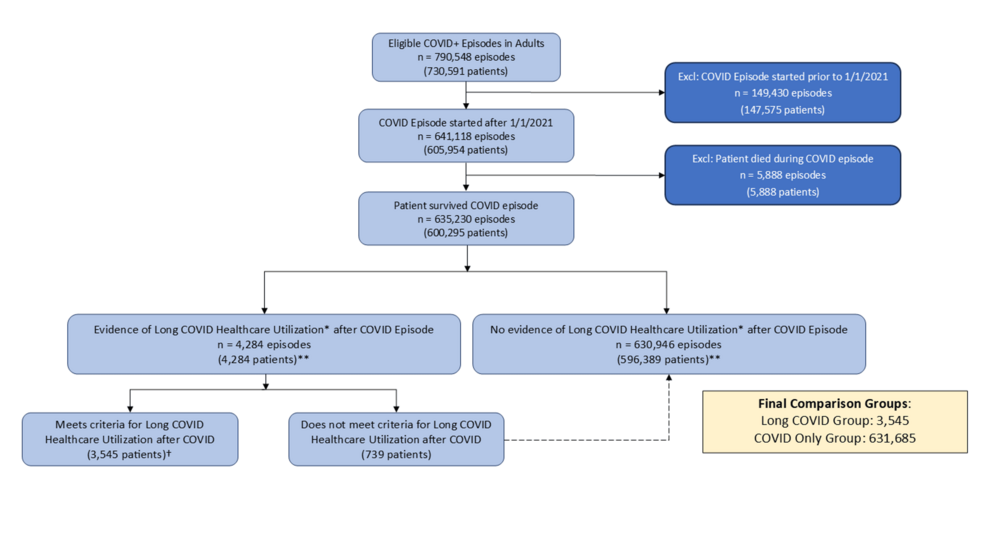
This was a retrospective cohort study of adult patients with documented SARS-CoV-2 infection (1/1/2021-6/30/2022) in a multi-site Northern California health system. Long COVID diagnosis was defined by at least one encounter with an associated International Classification of Diseases, Tenth Revision code and/or referral to Long COVID specialty care. Utilization outcomes included inpatient/outpatient encounters, laboratory/imaging/functional testing, specialty care referrals/encounters, and medication use. We used propensity-weighted difference-in-differences models adjusted for study month to compare outcomes between baseline and post-SARS-CoV-2 infection (Long COVID window).
Results
Among 600,295 patients with 635,230 SARS-CoV-2 episodes, 3,545 met criteria for Long COVID care-seeking. Long COVID patients had higher baseline utilization and greater increases in post-diagnosis utilization in adjusted analyses. After propensity weighting, these differences persisted and were consistent across the study period, particularly in cardiac and pulmonary care. Total encounters per year were 29.9 post and 14.1 pre (Long COVID) versus 17.7 post and 12.5 pre (NO Long COVID). Total annual ED visits per 100 patients were 65.1 post and 38.0 pre (Long COVID) versus 38.0 post and 32.0 pre (NO Long COVID). Annual hospitalizations per 100 patients were 10.5 post and 5.3 pre (Long COVID) versus 7.4 post and 5.5 pre (NO Long COVID).
Conclusion
Long COVID patients had higher healthcare utilization before and after diagnosis, with sharper increases across nearly all outcomes.

The Long Tail of Long COVID-19: Broad and Extensive Increase in Utilization Within an Integrated Healthcare System
Background: The impact of the emergence of Long COVID on healthcare utilization in a U.S. community setting remains underexplored. Objective: To examine the healthcare utilization of Long COVID patients compared with pre-COVID-19 era controls before and after SARS-CoV-2 infection within a large...
Abstract
Background
The impact of the emergence of Long COVID on healthcare utilization in a U.S. community setting remains underexplored.
Objective
To examine the healthcare utilization of Long COVID patients compared with pre-COVID-19 era controls before and after SARS-CoV-2 infection within a large integrated delivery system.
Methods
This was a retrospective cohort study of adult patients with documented SARS-CoV-2 infection (1/1/2021-6/30/2022) in a multi-site Northern California health system. Long COVID diagnosis was defined by at least one encounter with an associated International Classification of Diseases, Tenth Revision code and/or referral to Long COVID specialty care. Utilization outcomes included inpatient/outpatient encounters, laboratory/imaging/functional testing, specialty care referrals/encounters, and medication use. We used propensity-weighted difference-in-differences models adjusted for study month to compare outcomes between baseline and post-SARS-CoV-2 infection (Long COVID window).
Results
Among 600,295 patients with 635,230 SARS-CoV-2 episodes, 3,545 met criteria for Long COVID care-seeking. Long COVID patients had higher baseline utilization and greater increases in post-diagnosis utilization in adjusted analyses. After propensity weighting, these differences persisted and were consistent across the study period, particularly in cardiac and pulmonary care. Total encounters per year were 29.9 post and 14.1 pre (Long COVID) versus 17.7 post and 12.5 pre (NO Long COVID). Total annual ED visits per 100 patients were 65.1 post and 38.0 pre (Long COVID) versus 38.0 post and 32.0 pre (NO Long COVID). Annual hospitalizations per 100 patients were 10.5 post and 5.3 pre (Long COVID) versus 7.4 post and 5.5 pre (NO Long COVID).
Conclusion
Long COVID patients had higher healthcare utilization before and after diagnosis, with sharper increases across nearly all outcomes.
