Here is an updated/edited version of the
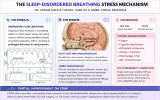
original AI summary of the UARS theory with links (most are to S4ME threads). I've also included an infographic and a talk by Dr. Denise Dewald on inspiratory flow limitation.
Abstract
This document outlines the
theory, primarily developed by
Dr. Avram Gold (medical director of Stony Brook University Sleep Disorders Center), that many "complex chronic illnesses" — including
Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS),
fibromyalgia (FM), and
Gulf War Illness (GWI) — are driven by a physiological stress response in the central nervous system (CNS) to obstructive sleep-disordered breathing.
The theory posits that the brain's limbic system becomes sensitized to
inspiratory flow limitation (IFL) during sleep following a significant physical or psychological stressor (e.g., infection, trauma, surgery, chemical exposure, etc.). This sensitization transforms previously benign IFL into a chronic, pathological stressor that perpetuates symptoms like fatigue, pain, cognitive impairment, insomnia and autonomic dysfunction.
This framework challenges the conventional understanding of sleep-disordered breathing by shifting the focus from apnea-hypopnea events and arousals to the neurological response to IFL. The evidence presented, drawn from clinical studies, case reports, and population data, suggests this mechanism is a cause for at least some cases of fibromyalgia and GWI, and warrants serious investigation for ME/CFS and other related conditions.
(
Note: Some of these diagnoses may represent multiple distinct disorders. For example, some GWI patients may have a true neurotoxic chemical injury — but many GWI cases don't fit that presentation, given features like dramatic symptom fluctuations over time.)
Why The Standard Paradigm Falls Short
A central tenet of this theory is that the current diagnostic paradigm for sleep-disordered breathing (SDB) is flawed and overlooks the primary driver of symptoms in many patients.
The Inadequacy of the Apnea-Hypopnea Index (AHI): The AHI, which measures complete and partial cessations of breathing,
correlates poorly with symptoms like fatigue and sleepiness (
1,
2). This is underscored by the fact that over 50% of individuals with obstructive sleep apnea (OSA, AHI ≥5) are asymptomatic. If apneas, hypopneas, and the resulting arousals were the primary cause of symptoms, a much stronger correlation would be expected.
The Central Role of Inspiratory Flow Limitation (IFL): The theory proposes that the crucial pathological event is not apnea but
IFL — the subtle, often inaudible
"fluttering" of the upper airway during inhalation. This includes snoring but also non-audible fluttering. Large-scale epidemiological data supports this:
snoring (a proxy for IFL) — not AHI — is the factor most strongly associated with subjective excessive daytime sleepiness* Two large sample size studies showed that increased IFL was independently associated with
subjective excessive daytime sleepiness* and
psychomotor vigilance task lapses, even after controlling for AHI, arousals, and other factors. However, IFL alone is not enough to cause symptoms;
one study comparing UARS patients to rigorously screened healthy matched controls found that even controls with no medical conditions, fatigue, or pain can have high levels of IFL.
*
A recent study identified that the Epworth Sleepiness Scale - which is used to assess daytime sleepiness - actually measures an uninterpretable mix of objective sleepiness and fatigue (which are uncorrelated symptoms in OSA patients).
A Two-Step Process
Dr. Gold's theory is not that inspiratory flow limitation itself causes these illnesses, but that the
brain's reaction to it does.
Step 1 — Pre-existing condition: An individual has a baseline level of IFL during sleep, which their brain does not perceive as a threat.
Step 2 — Sensitizing event: A significant stressor — such as an infection, physical/psychological trauma, surgery, or chemical exposure — activates the body's primary stress pathway, the hypothalamic-pituitary-adrenal (HPA) axis.
- The Sensitization Mechanism: This HPA axis activation leads to the sensitization of the limbic system (the brain's emotional and stress-response center). The hypothesis suggests this may occur via the olfactory nerve, which senses changes in nasal airflow and pressure and has direct connections to the limbic system. (During IFL, there are prolonged decreases in nasal pressure compared to non-flow-limited breathing).
- The Pathological Consequence: Post-sensitization, the brain begins to interpret the previously ignored IFL as a noxious, threatening stimulus. This triggers a recurring, nightly stress response that drives the diverse symptoms of chronic illness, from profound fatigue and widespread pain to autonomic dysfunction and cognitive impairment.
- Relevant supporting observation: A study by Dr. Gold of consecutive SDB patients at a sleep clinic identified an inverse relationship between AHI and symptoms like sleep-onset insomnia, headaches, and IBS, with UARS patients having the highest prevalence of these symptoms and patients with moderate-severe OSA having the lowest. This fits the theory: as frequency of apneas (complete/near-complete cessation of airflow) increases, exposure to IFL decreases.
Multiple lines of evidence support the connection between IFL and complex chronic illnesses.
Gulf War Illness: A Controlled Study and Treatment Trial
Fibromyalgia: Converging Evidence
The link between SDB and fibromyalgia is supported by evidence from multiple directions — physiological, epidemiological, and clinical.
- Upper Airway Collapsibility: A study by Dr. Gold found that female fibromyalgia patients had a more collapsible upper airway — comparable to female UARS patients — measured by the pharyngeal critical closing pressure (Pcrit), providing a physical basis for increased IFL.
- High Prevalence of fibromyalgia in OSA: A meta-analysis found a 21% prevalence of fibromyalgia in OSA patients (compared to a 1.78% prevalence of fibromyalgia in the general population).
- High Prevalence of OSA in fibromyalgia: One study found that when polysomnography was offered to consecutive female fibromyalgia patients in a rheumatology clinic. Of the 23 who agreed to testing, 100% had OSA — compared to ~17% in the general female population. Only 14 of the 23 (61%) had sleep-related complaints — lower than the >90% rate of sleep complaints reported in fibromyalgia patients in the broader literature, suggesting the participants who agreed to testing were not disproportionately those with sleep concerns.
- Symptom Resolution with Treatment: At least two independent case reports from different countries document the near-complete resolution of severe, long-standing fibromyalgia symptoms following treatment for OSA (one with CPAP, one with a mandibular advancement device). Critically, one report documented that alpha-delta sleep—an objective biomarker associated with fibromyalgia—disappeared along with the patient's symptoms after treatment.
Orthostatic Intolerance (OI) / Dysautonomia
The theory may also explain the different autonomic presentations between UARS and OSA, particularly with respect to
orthostatic intolerance.
- UARS and Hypotension/OI: One study found that 93/400 consecutive UARS patients at Stanford had low blood pressure (BP), and of those, all 15 who underwent tilt-table testing had orthostatic hypotension. By contrast, only 2/3,369 consecutive OSA patients had low BP.
- Mechanism of Divergence: A study found higher parasympathetic activity in UARS patients compared to controls, particularly during breaths with increased inspiratory effort — a possible mechanism for low BP and OI. By contrast, in classic OSA, recurrent hypoxemia and arousal-related pressor responses are thought to be major drivers of daytime hypertension. A case report documented a man with OSA who developed progressively worsening low BP and orthostatic hypotension symptoms after temporarily stopping CPAP, which resolved promptly with reinstatement.
Chronic Insomnia
Chronic insomnia — common in ME/CFS, fibromyalgia, and GWI — has been shown to be very strongly associated with SDB.
- In a study of chronic insomnia patients who believed their sleep problems were due to psychological, psychiatric, behavioral, or environmental factors, after excluding hundreds of patients with OSA signs/symptoms and risk factors, only 1/62 chronic insomnia patients who underwent polysomnography (PSG) did not meet criteria for OSA/UARS. Of the 40 final patients, 90% met criteria for OSA and 10% UARS (the prevalence of OSA in the general population is ~20%). In the same study, PAP treatment led to remission from chronic insomnia in a substantial proportion of patients.
Additional Population-Level Evidence
Beyond fibromyalgia, population-level data suggest OSA is associated with other conditions that overlap significantly with ME/CFS.
- Long COVID / PASC: A cross-sectional survey of ~25,000 US adults found that OSA was independently associated with all PASC symptoms tested, with effect sizes holding up well after adjustments for BMI, comorbidities, vaccination status, and socioeconomic factors. Most strikingly, treated OSA was not associated with elevated PASC risk. A separate multi-network EHR analysis of over 2 million COVID-positive patients found consistent elevated odds of probable PASC in adults with pre-existing OSA, though the association attenuated more after comorbidity adjustment, leaving confounding as a more open question.
- Bladder Pain Syndrome / Interstitial Cystitis (BPS/IC): A population-based cohort study found that patients with OSA had nearly 4× the risk of subsequently developing BPS/IC over a 3-year follow-up — and the adjusted hazards ratio (3.71) differed only modestly from the unadjusted one (4.43), even after controlling for fibromyalgia, IBS, CFS, depression, panic disorder, chronic pelvic pain, and other relevant comorbidities. BPS/IC is one of a cluster of conditions — including fibromyalgia, IBS, and ME/CFS — that frequently co-occur and are thought to share underlying mechanisms involving central sensitization.
A Unifying Framework
This theory provides a unifying framework that could explain many puzzling aspects of ME/CFS and related disorders.
- The Hypermobility Connection: It can explain why people with hypermobility/EDS are more likely to develop ME/CFS, fibromyalgia, and related disorders: lax connective tissue means a more collapsible upper airway. A meta-analysis found that patients with EDS and Marfan syndrome were ~6 times more likely to have OSA than the general population. A parallel cohort study of EDS patients and matched controls found that the impact of EDS on AHI was comparable to that of a 11 kg/m2 BMI gain.
- Diverse Triggers: It can account for how any type of stressor — not just infections — can trigger an identical syndrome by focusing on HPA axis activation as the common pathway to sensitization.
- Symptom Variability/Fluctuations: It can account for both gradual and sudden onsets, and why symptoms in ME/CFS and related disorders often fluctuate — sometimes significantly within the same day or hour. It also provides a plausible explanation for remissions, relapses, and why recovery is more likely early on, especially with rest/pacing (stress response less ingrained). It can even account for "mind-body" recoveries in some individuals, if those approaches are sufficient to modulate the UARS stress response.
- Post-Exertional Malaise (PEM): In this theory, PEM can be understood as a manifestation of a dysfunctional CNS stress response. Exertion — physical, cognitive, emotional, or sensory — acts as an additional stressor on an already over-taxed system, triggering a crash. This aligns with observations that CNS depressants (e.g., benzodiazepines, dextromethorphan) can sometimes prevent or reduce PEM, and that PEM severity does not always correspond to energy expenditure, but seems to track more closely with how much "stress" — positive or negative — an activity or stimulus places on the system.
- Partial Efficacy of Treatment: It can explain why CPAP/BiPAP often provide significant (~35-50%) but incomplete relief. While PAP reduces IFL, the device (pressure, mask) can act as a new stressor on a highly sensitized nervous system, limiting the degree of recovery. More curative treatments may involve surgery or, for some, nervous system regulation techniques that aim to desensitize the stress response itself.
"I think of flow limitation as a really important thing to look at when you're looking at a PSG [polysomnogram] and deciding: is this a normal study or not? Spoiler alert: just about everyone who's referred for a sleep complaint does not have a normal study. After thousands of sleep studies, I have yet to see an actual normal study [i.e., no flow limitation during non-REM sleep] in someone who was symptomatic. The only normal studies I've seen are people referred because they needed a sleep study for bariatric surgery, or because they work in transportation...Oh, and there was one guy sent by his cardiologist because he developed atrial fibrillation — but he had rheumatic valvular disease." — Denise Dewald, MD
Physiology/physics of IFL (and Pcrit) is discussed at 5:45.